Shoulder Injuries
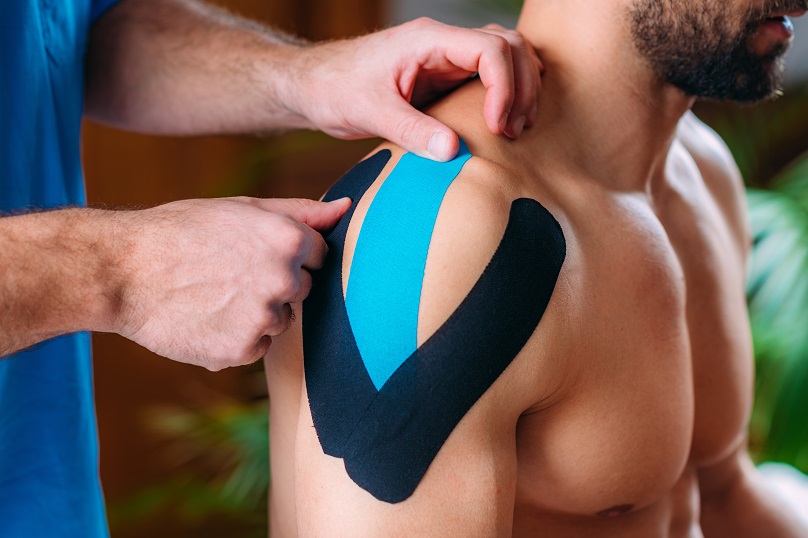
The first step in helping someone with shoulder pain is to work out where the pain is actually coming from. True shoulder pain usually presents with a difficulty with movements like reaching overhead or behind the back. However, sometimes the neck can refer pain to the shoulder which is usually more of an ache or neural pain without the restriction of shoulder motion.
True shoulder pain can then be classified into an acute or non-acute injury.
Acute
Acute injuries to the shoulder often involve a traumatic event like a fall onto the hand or point of the shoulder. This can happen in a sporting environment or with a trip and fall. Rotator cuff tears, AC joint sprains, shoulder dislocations and fractures can all result from a fall. These injuries are usually fairly easy to diagnose and will typically present with pain and weakness when attempting to lift the arm. When necessary we will use x-rays and ultrasound scans to help determine the exact location and severity of the injury. Often simple measures like immobilization followed by a rehab program will provide successful outcomes for these acute injuries. Occasionally surgery will be required.
Non-acute
Non-acute shoulder pain develops more slowly. Chronic shoulder pain can severely affect quality of life - you may have trouble sleeping on your side, lifting the arm overhead when washing your hair or when reaching behind your back when getting dressed. There are 3 main non-acute shoulder pathologies – shoulder tendonitis, frozen shoulder and calcification. With all of these conditions there is often pain beneath or around the tip of the shoulder so differentiating between these conditions can be challenging. Frequently there can be overlap and persons can experience pain from multiple pathologies.
Our approach at RP is to first rule out frozen shoulder (adhesive capsulitis) as it is usually the most obvious condition. With a frozen shoulder restriction/stiffness is often a significant symptom and this can be associated with several movements like reaching behind the back or overhead. There are 2 stages with a frozen shoulder – ‘freezing’ and ‘thawing’. A frozen shoulder will often progress and get progressively worse in terms of pain and movement restriction during the freezing stage. Often in the very early stages when stiffness is not so obvious the diagnosis may be missed. It can take anywhere between 1-2 years for a frozen shoulder to fully recover. There can be considerable muscle tension around the joint as well as into the neck and we find that gentle physio techniques can provide symptomatic relief for this. It can also be beneficial to start some therapeutic exercise to maintain motion in the joint when first diagnosed and then more strenuous stretching and strength work can commence as the shoulder begins to naturally ‘thaw’.
With shoulder tendinopathy there can be some stiffness with movements of the arm but not to the same extent as seen with a frozen shoulder. There is often a painful arc of motion and a kyphotic or rounded shoulder posture. The supraspinatus tendon is most frequently affected. The cause of shoulder tendinopathy may be as a result of repeated compression against the overlying acromion or simply overuse after doing too much too soon. Our treatment approach for shoulder tendinopathy focuses on firstly correcting for any stiffness and postural faults present. We believe that this helps ‘centralize’ the shoulder joint reducing tendon compression and irritation. Specific massage techniques are also useful to provide some pain relief and kick-start healing within the tendon. Strong shoulders are generally healthy shoulders so we will also work to ensure the muscles around the shoulders are balanced and working correctly. The shoulder can be compared to a tent – all of the guy ropes need to be pulling at the right tension for the tent to sit correctly.
Shoulder calcification can cause severe pain and it is this nature of pain that can often help differentiate it from other shoulder pathologies. Shoulder calcification is characterized by the deposition of calcium deposits in the rotator cuff tendons. The cause of formation of these deposits is unknown. In over 90 percent of cases they disappear spontaneously but this may take up to 1 year. When the calcium deposit is causing impingement physiotherapy may help alleviate symptoms by correcting any stiffness and weakness creating a more ‘balanced’ position for the shoulder. If a ‘wait and see’ approach and physio fail to provide relief surgical intervention or needle aspiration can provide undertaken.